Since 2000, the methods of diagnosis and treatment of macular degeneration have exploded. No longer is the disease guaranteed to progress and cause blindness.
What is Macular Degeneration?
 Macular degeneration is a disease of the part of the retina that provides central or "detail" vision. This central part of the retina, known as the macula, allows the eye to read numbers and letters and recognize faces.
Macular degeneration is a disease of the part of the retina that provides central or "detail" vision. This central part of the retina, known as the macula, allows the eye to read numbers and letters and recognize faces.
The findings of macular degeneration differ depending on the type:
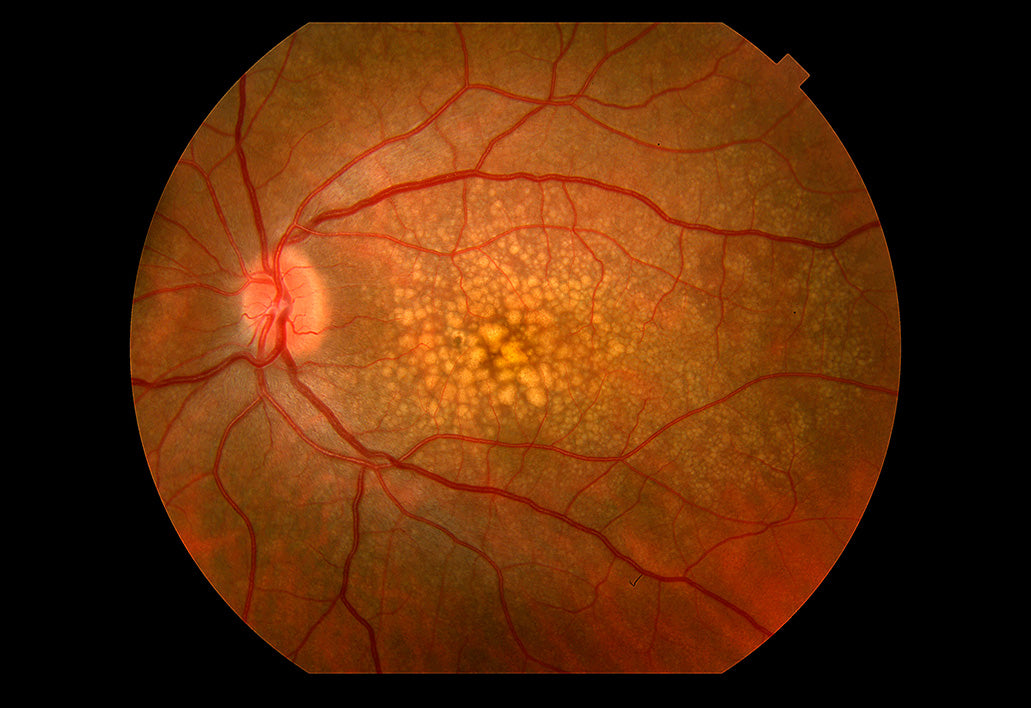
- Dry Macular Degeneration (Atrophic Macular Degeneration): Notable for atrophy or thinning of the macula as well as the formation of collections of lipofuscin in the macula, which are known as drusen.
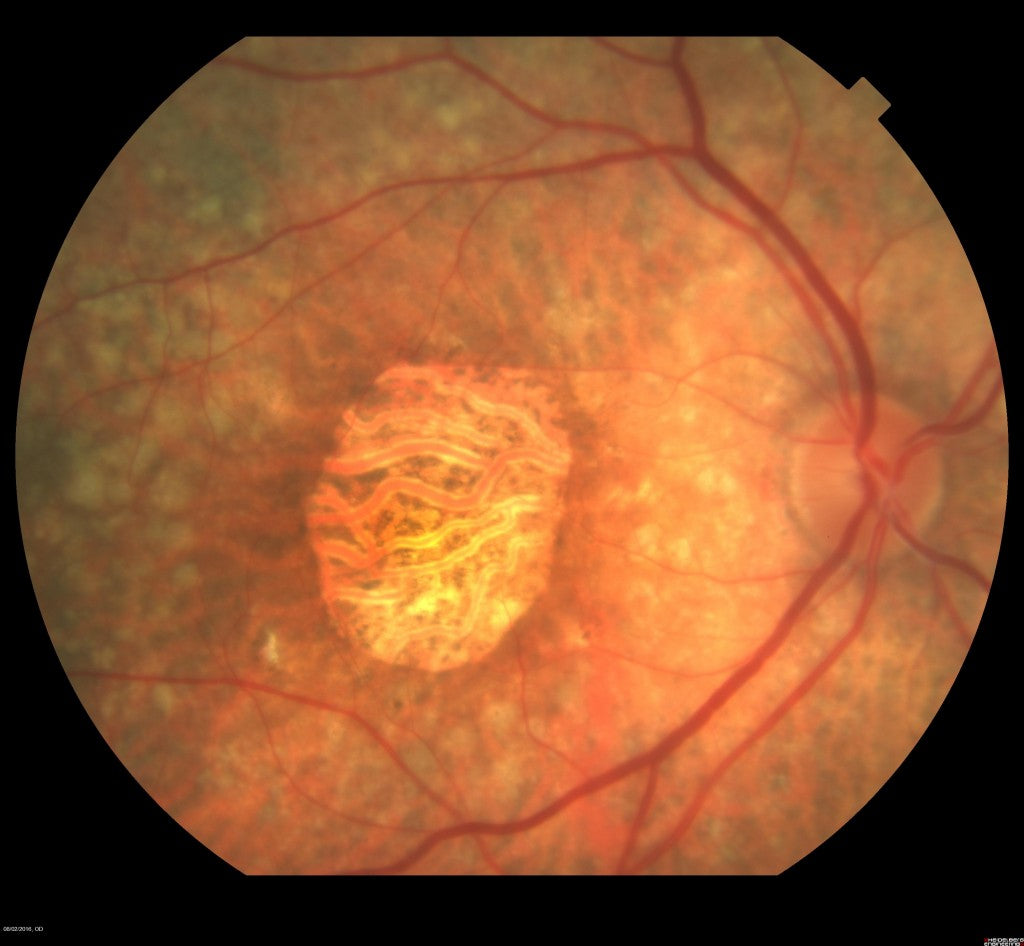
- Wet Macular Degeneration (Exudative Macular Degeneration): Characterized by the formation of abnormal blood vessels (neovascularization) beneath the retina, which results in bleeding, leakage of protein, and rapid damage to the retina if left untreated.
The diagnosis and treatment of macular degeneration have improved since 2000 due to three major factors:
1. Diagnosis:
Previously, doctors would assess using a direct ophthalmoscope or sometimes indirect ophthalmoscopy. If there were suspicions of the macular degeneration progressing, for example dry macular degeneration becoming wet macular degeneration, doctors would perform fundus photography or sometimes fluorescein angiography.
However, the advent of OCT (ocular coherence tomography) [see image below] has made the process of evaluating the degree of macular degeneration rapid, easy and painless.

2. Prevention:
The National Eye Institute published the first AREDS (Age Related Eye Disease Study) in 2001, AREDS 2 in 2014, and other studies have been published since that document the benefit to high dose ocular nutritional supplements in slowing the progression of disease. Additionally, research now proves that there may be a genetic component to many cases of macular degeneration. Rather than be a negative, this has encouraged family members of patients who have macular degeneration to seek more frequent and early care.
3. Treatment:
The recent development of medications that cause the neovascular blood vessels of wet macular degeneration to recede (Lucentis, Avastin, Eyelea, others) mean that the devastating effects of wet macular degeneration may be halted. The downsides to these medications thus far is that they need to be repeatedly injected into the eyeball, and they have added a huge new medical cost that previously did not exist. However, the fact that they have the ability to stop blindness has created a hopeful quality of life for those affected.